Stanford researchers estimated that 9% of the U.S. contracted COVID-19 by July 2020, in a paper recently published in The Lancet. As the country reopens, researchers say both vaccines and public intervention are needed to prevent that number from multiplying.
To those advocating for a herd immunity approach, the study highlights a long path ahead. For the strategy to succeed, experts generally agree that 60-70% of our population would need to develop immunity.
Shuchi Anand, the study’s lead author and professor of medicine, said her team’s work presents the first national study of COVID-19 infections. To arrive at her 9% infection estimate, she measured virus antibodies in dialysis patients, who undergo weekly blood sampling.
Anand said that there have been some concerns about the accuracy of the results.
“Concerns with dialysis patients are bidirectional,” she said. “They are older and less healthy, so they may be more susceptible. They are also more likely to be cautious and less exposed to the workplace.”
Speaking to the net bias of the data, Anand said that “9% is more likely to be an overestimate.”
Research at Stanford attributes these low numbers to the shelter-in-place orders in March and May.
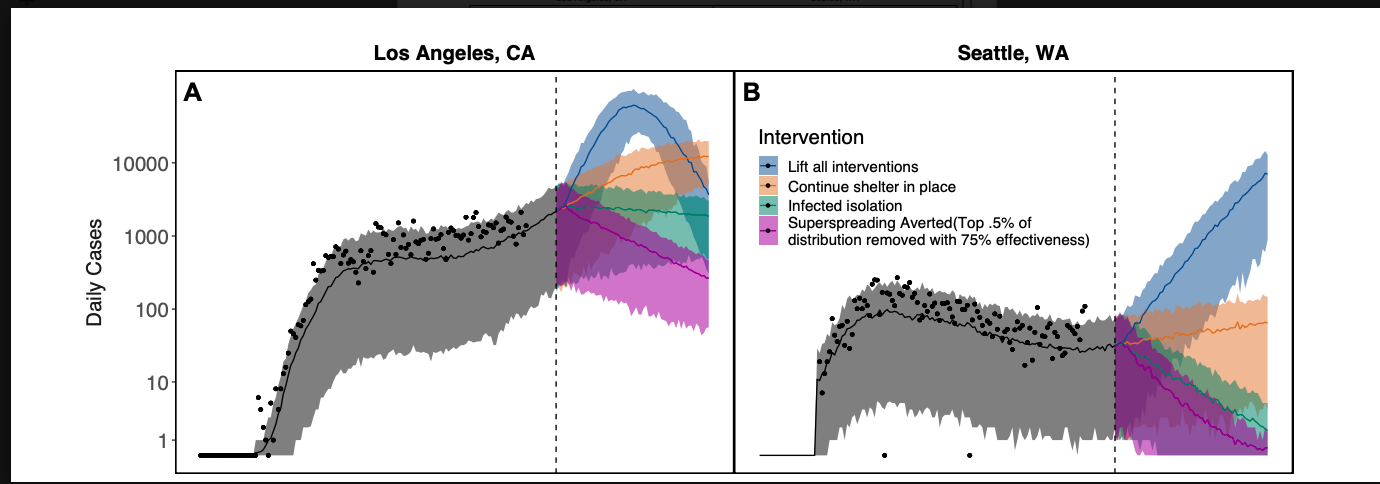
“Before the interventions, each person was infecting an average of two other people — in many cases, five or even 10 people,” biology professor Erin Mordecai said. “After the early interventions, there was a dramatic decline in new cases, with each person infecting an average of 0.8 people.”
Researchers say that continued intervention could curtail the virus. Alexander Becker, a postdoc working with Mordecai, said that keeping the infection rate low would decrease new cases, bringing the pandemic under control.
As the nation weighs reopening, Becker said simply averting superspreading would be highly effective.
“Superspreading plays a very important role in the current outbreak, he said. “It’s estimated that 10-20% of infected people account for 80% of SARS-CoV-2 transmissions.”
“We simply need to chop the tail end of highly infectious patients. By limiting the sizing of indoor gatherings, we make it impossible for superspreading to infect dozens of people in a 24-hour sitting.”
As many hope that a vaccine will return life to normal, some researchers say social restraint might be the new normal. Even if a majority take the vaccine, Stanley Deresinski, professor of medicine, said, it may not offer complete immunity.
“The FDA requires the vaccine to be 50% effective — that means even if 50% of people take it, you’re left with an effective 25% immunity rate,” Deresinski said.
Deresinski also pointed to delayed distribution and short-term protection from the vaccine as potential challenges.
Speaking to the combined effect of these obstacles, Deresinksi said “COVID-19 might be with us forever. The Spanish Flu is still with us 100 years later.”
Contact Yash Dalmia at yashdalmia ‘at’ stanford.edu.